It’s inevitability by demography.
The entire population of the United States is right around 330 million. By 2030, even the youngest of the Baby Boomers — a cohort that makes up about 22 percent of the population — will top age 65. By 2035, according to the Census Bureau, there will be more adults 65-plus than children under 18.
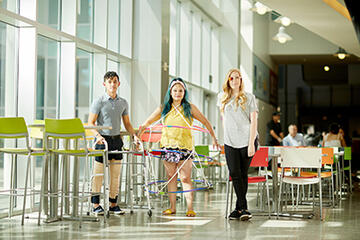
Health Care at Every Corner of Campus
UNLV's commitment to studying and improving health care goes beyond the School of Medicine. Disciplines all over campus are involved in improving the industry, from every angle.
Aging, and all the physical and cognitive problems that go with it, will be one of the dominant social concerns of the coming years. And it’s not just a graying America that will challenge us: The veteran population right now is around 19 million, including about 4 million people with physical or mental disabilities. Overlapping the health of those populations is a society that is starting to increasingly focus on general wellness and preventive medicine, all in a country that spends 18 percent of its gross domestic product on health care compared to 11.5 percent, on average, in other high-income countries.
But addressing our 21st century health concerns extends far beyond doctors visits and prescriptions. For Attila Lawrence, our built environment must change too.
“Human well-being and human health has a lot to do with not only medical attention, but it has lot to do with behavior,” the interior architecture and design professor said. “But behavioral therapy cannot be successful without understanding the role of the environment. The best care, it doesn't matter what it is, takes place in your home environment.”
That need is what drove Lawrence to create the School of Architecture’s healthcare interior design master’s program in 2017. More than just designing hospitals and doctor’s offices, health care interior design aims to build out spaces that accommodate individuals’ needs. It can be anything from lowering counters for people in wheelchairs; to installing softer materials for flooring and counters with rounded corners and discreet grab bars for those in danger of falling. Those are obvious, simple examples, but often the practice can be as subtle as changing colors and patterns to highlight differences in elevation stop or lesson a schizophrenic episode.

A focus on health care fundamentals
The discipline occupies such a rare space that only a handful of other universities offer health care interior design, and none in the West. Similar programs can be found at Clemson, Texas Tech, Kent State, Florida International University, University of Virginia and Boston Architectural College.
Yet people, Lawrence notes, spend about 90 percent of their lives indoors — even the most nature-oriented among us. Those environments impact your mood: how calm you are, how agitated you are, even how much alcohol you might drink.
That fact gnawed at Lawrence. Friends would share pictures from design magazines of rooms they wanted, but he knew wouldn’t be good for them. Then there was an educational event at The Cleveland Clinic’s Lou Ruvo Center for Brain Health. It emphasized the importance of nutrition and exercise but never considered the environments that help people achieve those goals.
So Lawrence met with Dr. Dylan Wint, a Ruvo neurologist and psychiatrist, to start what would be a fruitful partnership with UNLV. Wint consulted with Lawrence on forming a curriculum — one that still includes students working closely with the Ruvo Center, presenting on various design issues up to three times a semester there.

Gaining unique perspective on health needs
Dak Kopec, who developed and launched the specialty at Boston Architectural College, was recruited to UNLV to help elevate the program here.
At the outset, he found UNLV interior design students already versed in health care design thanks to Lawrence incorporating the subject into undergraduate classes.
“At the end of [my] interview when I saw the student work — these students were already translating research into design,” Kopec said. “Just simple things like, how do you design differently for an ischemic stroke versus a hemorrhagic stroke? It hadn’t seen that in a lot of programs. [Other] students don't know. Most of them don't know the difference between the dementias, but these students did at UNLV.
“This was a starting point that is much higher than what I'm used to.”
Part of that curriculum involves Kopec’s Built Environment and Human Health class, where students simulate various conditions and disabilities. For macular degeneration, they wear swim goggles covered with purple dots on the lenses. For osteoarthritis, boards are strapped to a student’s leg to force them to move with an unbending knee. And hoops draped in fabric simulate the difficulties someone with morbid obesity faces walking from the Paul B. Sogg Architecture Building to the Student Union, buying lunch or coffee, using the bathroom, and then returning.
“Those are things that they're not used to doing because we're used to just creating the picture of this,” Kopec said. “I have architecture students who will take this course because they find it fascinating, but I never get them again. With the interior students I can hear [the experience] in their process.”
A key part of the training is designing holistic projects that address a host of needs. That can mean a theoretical home for a multigenerational family with multiple issues, or it could mean designing spaces for specific concerns.
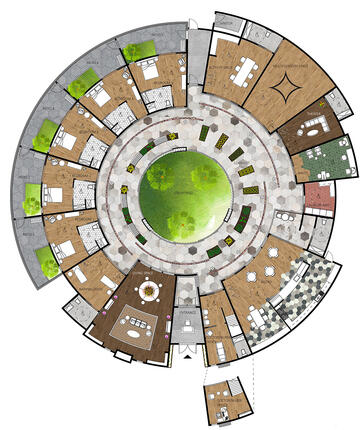
In the center, an open courtyard is easily accessed “so they're going to the outside but it's still a controlled environment,” Odette said. “But we hid the exit doors [in the main part of ] the building so they would not try to [wander away].”
Those are the types of research-informed design solutions the School of Architecture’s graduates will need to be able to produce in the coming years. Not only will they be crucial for patients from a purely health care standpoint, but the demand for those skills will explode in the near future.
Between 2005 and 2015, Nevada’s 65-plus population increased by more than 50 percent, and the number of people in the state 85 and older has grown 75 percent in the last decade, and instances of Alzheimer’s are expected increase at least 14 percent in every state by 2025.
All of that adds up to a field that should see a surge in demand, both in new construction and in repurposing existing structures to meet new demands.
“The younger, many of them are moving back with their parents, which is good in a way the younger person doesn't feel cut off from the rest of the world,” Lawrence said. “Economically, it's a gold mine because the home will have to be suitable for everybody. Some renovations will have to be done because a home that was built 30 to 50 years ago lacks all the things that will make it user-friendly for all members of a multi-generational family.
“It will also have a lot to do with not only social sustainability but environmental sustainability, simply meaning that we are keeping [buildings]. So we're dealing with sustainability at different levels, we’re dealing with economics, we're dealing with a deeper sense of social responsibility, but also dealing with spirituality in some sense.”