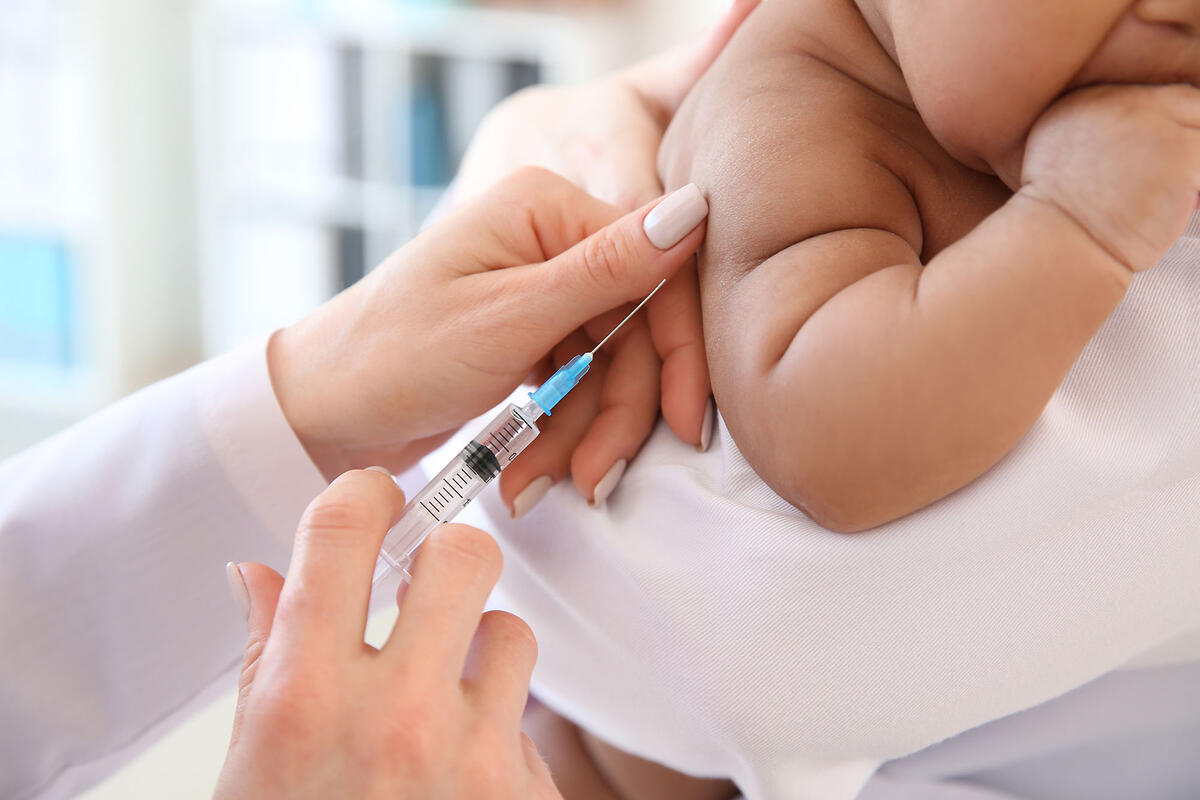
One of the greatest medical breakthroughs of modern civilization — vaccinations — has become increasingly controversial in recent years.
Parents are urged to give their children vaccinations soon after birth and throughout adolescence. And though vaccines are usually part of a routine doctor’s visit, some parents question their value.
Johan C. Bester, UNLV School of Medicine Bioethics Director, said vaccinations, quite simply, protect us from vaccine-preventable diseases that are extremely dangerous.
Outbreaks of preventable diseases have been occurring nationwide and are steadily increasing. From 2017 to 2018 — the course of just one year — the number of measles cases reported to the Centers for Disease Control and Prevention (CDC) more than tripled from 120 to 372.
In 2019, confirmed cases have already surpassed last year’s total, with 555 reported cases to date. This is the second-greatest number of cases reported in the U.S. since measles was eliminated in 2000, according to the CDC.
To understand why vaccine-preventable diseases have been increasing in numbers, we caught up with Bester, who addressed the role of vaccinations and how they keep Americans healthy.
Why are vaccinations necessary?
The role of vaccinations can be boiled down to one simple thing: vaccinations protect children against harmful, infectious diseases. There are short- and long-term complications for children who are not vaccinated. Contracting measles, for example, can lead to frightening complications including pneumonia, hospitalization, and death. Measles can compromise a child’s immune system for up to 3 years which causes other infections, and it can also affect your brain. It’s a devastating illness, but the measles vaccination is extremely effective. A single shot is 92 to 95 percent effective at preventing measles, and if you get the recommended two shots, it is 99 percent effective — two vaccines reliably protects a child against measles.
The secondary role of vaccinations is the obligation to society. We owe children vaccinations. It is something that undoubtedly protects them from harmful diseases. It’s something we should be doing unless we have a good reason not to.
How do vaccinations protect others?
Not everybody can be protected through vaccination. Some individuals are unable to receive vaccinations due to age, life-threatening allergies, or other health problems. Those who are able to safely receive vaccinations should do so, because it prevents dangerous diseases from spreading through the population and infecting those who cannot receive the vaccine. This is called the herd effect. With measles, the vaccine is not effective for children under 9 months, and in the U.S. the first vaccine is given at 12 months, so they’re susceptible to contracting the disease for that period of time. Also, immunocompromised individuals cannot be vaccinated and are susceptible to measles.
We need to have an extremely high rate of vaccinations — 95 percent — because the more refusals we have, the more the above-mentioned individuals cannot be protected. If we vaccinate at lower rates, it creates pockets of vulnerability in the population where disease outbreaks can happen and spread. Nationwide, we hover around 90 percent mark for 1 dose of measles vaccine depending on which year you look at. Some states fall well below the 90% mark. It’s close to where we want to be, but not quite there.
Is there a link between vaccines and autism?
The question has been studied and continues to be studied over and over again. There have been over 45 studies of this question involving millions of children, and it is clear that there is no link between the measles, mumps, and rubella (MMR) vaccine and autism.
In the 1990s, a research study proposed a link between the MMR vaccine and autism, and that news exploded in the media. The study was found to be fraudulent — among other things, data was made up. On its face the study also was not scientifically compelling: it used case studies of 12 children and then asked parents to recall symptoms from long ago, introducing a lot of bias and chance. The paper was retracted by the journal and completely discredited, but the idea of a link has persisted among those skeptical of vaccines.
Why do some people believe that vaccinations are harmful?
There are many reasons, but one reason is the false information about vaccines that can easily be found on the internet. If you look at this misinformation, you’ll find a variety of suggestions for why vaccines are unsafe. If one presents evidence that this information is false, then another reason why vaccines are unsafe is offered. This is the idea of shifting hypotheses.
If you prove that we’ve studied and found that there’s no link between vaccines and autism, then it shifts to, “What about the mercury in vaccines?” Once you tell them that the mercury been removed from all childhood vaccines except the flu shot, and the thimerocel in the vaccination is not the harmful kind of mercury, then it shifts to: “Isn’t it dangerous to overwhelm a child with several shots all at once?” Well, a child who crawls over the floor comes into contact with millions of bacteria and antigens. So receiving five antigens in an injection is not anything strange to the immune system, and they won’t cause an infection like the measles virus or a bacterial infection can. Science has addressed all of these concerns, but some will not be convinced.
Some people are also skeptical because they think there’s a conspiracy between vaccine manufacturers, government, and the medical establishment. But childhood vaccines are not that profitable, and they’re highly subsidized by the government. It is hard to see how such a conspiracy would be kept secret, and it is hard to see what the aim of such a conspiracy would be.
Is it possible for vaccine-preventable diseases to make a resurgence?
Absolutely — that’s what happened in the U.K. They eliminated measles before we did, then came the fraudulent research study that proposed a link between the MMR vaccine and autism. There was a huge autism scare and vaccine rates dropped into the 80 percent range. As a result, measles came back, and in 2008 the disease was declared endemic to the U.K. More refusals will lead to more outbreaks, which could cause currently eliminated diseases to become endemic in the U.S. once again. One of my biggest concerns is that measles will come back in the U.S., and we see more and more outbreaks in recent years.
What do you think can be done to increase the rate of vaccinations?
We need to work to rebuild trust between the medical establishment and people who are afraid of vaccinations. I think public education and public messaging could help, and we need to clamp down on erroneous or wildly inaccurate messages regarding vaccinations.
The best thing we can do is to try and foster trust relationships between community medical providers and parents. It has been shown, convincingly, that if parents have a trusting relationship with their primary care provider and other healthcare professionals, that relationship can help parents resist anti-vaccination messaging.
About Johan Bester
Johan Bester is the Director of Bioethics at UNLV School of Medicine and an assistant professor in the department of Family Medicine. Before arriving at UNLV, Bester taught and practiced family medicine at the University of Calgary. He also completed a year of fellowship training in clinical ethics at the Cleveland Clinic in Cleveland, Ohio, and spent an additional year on staff as a clinical ethicist. His work focuses on the ethical aspects of vaccination, pediatric ethics, justice, best interests, medical decision-making, ethical theory, and related concepts.