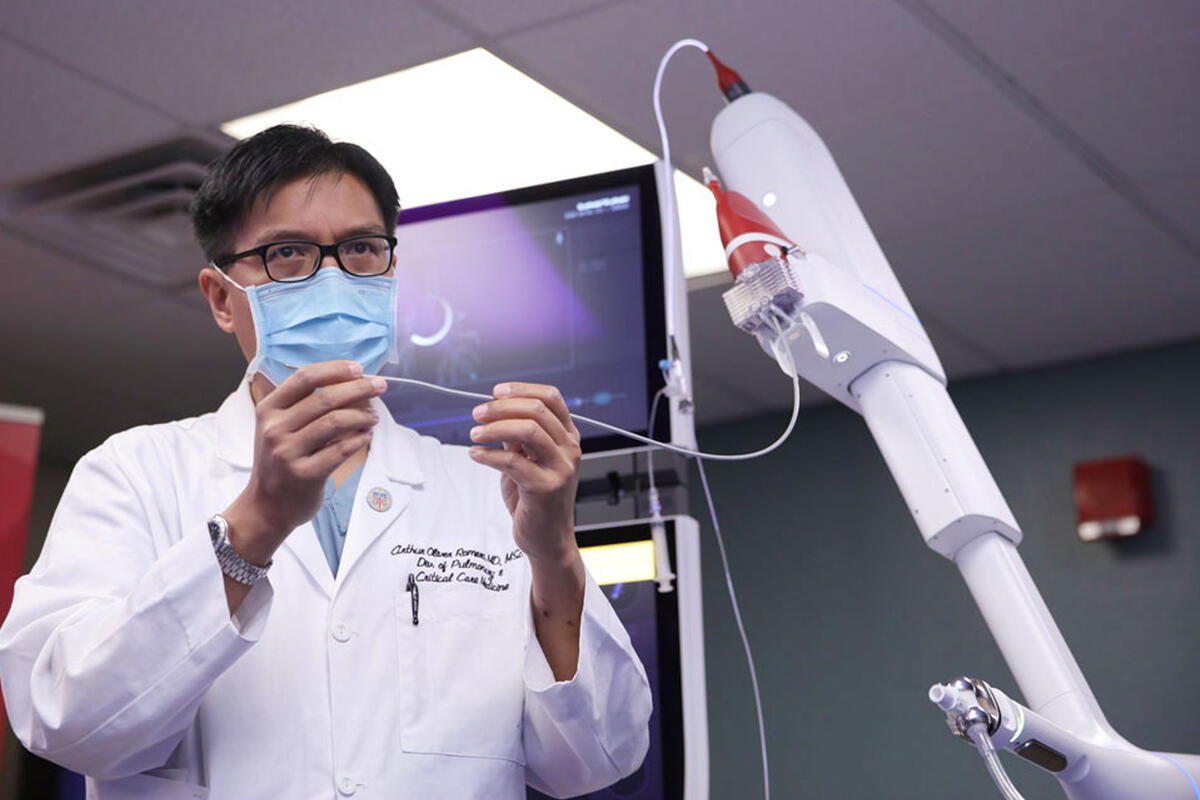
Dr. Arthur Oliver Romero of UNLV Medicine received advanced fellowship training to use a robot-assisted biopsy platform, called ION, that was newly acquired by University Medical Center.
In June, he may well have saved a life with it.
Romero used ION to diagnose a patient with early-stage lung cancer. Diagnostic tissue from the hard-to-reach lesion was collected through robotic bronchoscopy and this information was given to a surgeon. Less than two weeks later, the patient underwent surgery to remove the tumor.
“That patient’s lung cancer is now gone,” Romero said. “We got it out before there was any evidence of spread.”
UMC is the only hospital in the state that uses ION. The system provides new levels of precision compared to manual biopsy techniques. It has an ultra-thin, easily controllable catheter that can bend 180 degrees in all directions. Doctors can use the catheter to navigate through the lung to reach nodules in any airway segment. It's more precise and safer for patients.
Lung cancer is the leading cause of cancer deaths, accounting for one in four cancer cases. More than 130,000 people die annually from lung cancer, which is more than the combined deaths from colon, breast and prostate cancers.
Romero honed in on lung cancer during a combined three-year postgraduate pulmonary critical care fellowship between 2007-2010 at University of California San Francisco-Fresno. He was a pioneer in Nevada, using advanced biopsy techniques to access difficult nodules in the lung, but he knew there were more patients that needed an even higher level of care.
With support from a UNLV grant, he went back to UCSF in 2019 for a year-long advanced fellowship to learn minimally invasive procedures to help patients with lung cancer and other advanced lung diseases.
Armed with better skills and broader experience dealing with the most complicated patients, Romero is now building the first interventional pulmonology program in Nevada. He is poised to help not only patients with lung cancer but other forms of advanced lung disease.
“We’re taking a big step forward for the people of Nevada,” Romero said. “People will be able to get world-class treatment right at home.”
Dr. Angelica Honsberg, who heads the pulmonary critical care division for the Kirk Kerkorian School of Medicine at UNLV says the new interventional pulmonology program at UMC will make a significant difference in lung disease care in Southern Nevada.
“Historically there has been a gap in lung cancer care in our area, with many residents being diagnosed at an advanced state of disease and not having consistent access to more advanced interventions," she said. "The new interventional pulmonology program, created through the joint efforts of the Kirk Kerkorian School of Medicine and UMC, offers Southern Nevada residents options for both lung cancer and severe emphysema treatment that they previously would have had to travel elsewhere to have. Our department is confident that being able to offer more options to Southern Nevadans will improve both quality of life and survival.”
Romero, who still must spend much of his time treating COVID-19 patients, is optimistic about the impact improved technology like ION, and other new procedures and treatments such as special valves that allow for treating those with emphysema without collapsing parts of the lung, will have locally.
“Without UMC acquiring the most advanced equipment available, I would not be able to offer the best care to many of our lung cancer patients,” he said.