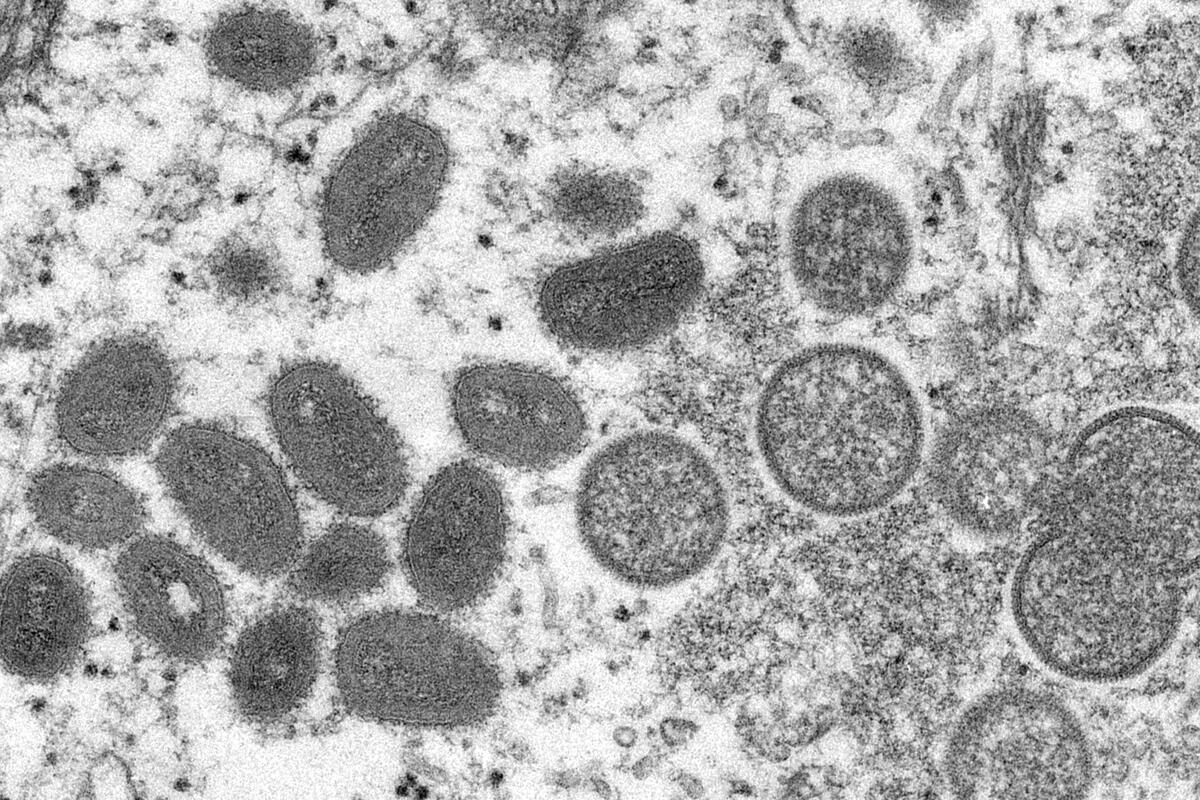
Our nation's shared experience with life-altering infectious diseases continued into its third summer in 2022, with monkeypox now joining coronavirus as the latest threat to public health.
By now, we’re all well aware that monkeypox is spreading around the world, including here in Nevada. The World Health Organization declared the spread of monkeypox a global public health emergency in the last few weeks, and data from the CDC shows that the U.S. now has more cases than any other country.

As of Sept. 1, there are more than 150 confirmed cases in Southern Nevada. While that doesn’t sound like much in a community of more than 2 million residents, the fact it’s in Nevada at all – and that numbers are rising – is enough to draw the attention of public health experts.
To learn more about monkeypox — what it is, how it spreads, how to protect yourself, and who needs to get vaccinated — we spoke with UNLV infectious disease expert Brian Labus. Labus, an epidemiologist and professor in the School of Public Health, has been an integral part of Nevada’s public health response to the COVID-19 pandemic and is a go-to source for media worldwide on infectious diseases.
What is monkeypox and how does it spread?
Monkeypox is a viral infection that causes a fever and a rash of pimples or blisters. It spreads mainly by skin-to-skin contact, typically during sexual activity. It can also be spread through a respiratory route, but it requires prolonged face-to-face contact. It’s not something that is going to spread during your daily activities or in a classroom.
Monkeypox has been around since the 1970s, primarily in west and central Africa. Why did it just recently become a concern internationally, including here in the U.S.?
The outbreaks of monkeypox we have seen in Africa over the past half century have typically occurred in rural areas. Rodents are the likely carrier of this virus, and people in rural areas are more likely to come in contact with the rodents. There was a small outbreak in the U.S. Midwest in 2003, when pet prairie dogs – infected after being housed near rodents imported from Ghana – came in contact with humans.
Similar to Ebola, the presence of monkeypox didn't concern the international community until it started to spread in urban areas, with outbreaks often fueled by sexual contact. Once the outbreaks were occurring in urban areas, international travel made monkeypox something that could easily jump borders, which is what we have seen over the past few months.
With that person-to-person spread across borders, the World Health Organization declared monkeypox to be a pandemic. In doing so, they were stating that it would require international cooperation to get this under control, something that wasn’t necessary when it was a small outbreak in a remote, rural community.
How likely is monkeypox to spread through normal daily activities (going to the store, sitting in a classroom or restaurant, etc.)?
Luckily, this isn’t something that spreads through normal activities in the same ways that COVID or influenza do. For example, you’re not likely to be exposed while standing in line at the grocery store, taking an elevator, or sitting in class.
Though it’s possible that members of the campus community will test positive for the virus, it won’t come from a classroom or workplace exposure.
How does monkeypox present itself, and what should people do if they think they may have it?
The characteristic sign of monkeypox is a pimple-like or blister-like rash that frequently starts in the genital area. It can also occur on the other parts of the body, often on the extremities. Like many other diseases, the rash may be preceded with vague signs and symptoms like fever, fatigue, sore muscles, and a headache. Not everyone has these, and rash can develop without them or even before they start. The rash can last for 2-4 weeks, and you are infectious until the scabs that eventually cover the rash fall off.
If people think they have monkeypox, especially if they have been recently exposed to someone with it or are part of a high-risk group, they should seek medical care for proper diagnosis and treatment.
How can people best protect themselves from monkeypox?
Your individual risk is what will tell you what you need to do to protect yourself.
The group with the highest risk is people who have had close contact with those infected with monkeypox. These people should get vaccinated as soon as possible after the exposure to reduce the risk of infection or serious disease.
Another group with an elevated risk is men who have sex with men (MSM). Over 95% of the cases in the United States have been identified among MSM and a high percentage of the cases have occurred in men who have had multiple, one-time sexual partners. For this group, vaccination can reduce the risk of infection, and so can behavior change. Skin-to-skin contact still occurs even with condom use, so even practicing traditional safe sex methods doesn’t really reduce the risk of monkeypox. While it isn’t easy to get people to change their behaviors, a recent CDC study found that about half of MSM reported reducing their high-risk behaviors to protect themselves from exposure.
The lowest risk group is people who do not fall into these other two groups. Because the risk for this group is low, there are no special precautions recommended at this time.
Monkeypox cases are rising in Southern Nevada, which - given the ebbs and flows of the COVID-19 pandemic - has caused some concern. Should we be worried?
Everybody is looking at monkeypox through the lens of COVID, so there is naturally going to be a lot of concern. Monkeypox is a very different disease, as it doesn’t spread as easily between people. It spreads more slowly in the community and deaths are very rare. A vaccine and treatments have also been available before the recent outbreak.
Most people fall into the low risk category, and for people at higher risk, there are steps that can be taken to reduce that risk – including vaccination. As with most diseases, we should have a healthy respect for monkeypox, but there is no reason to fear it.
One of the biggest challenges we face is a limited vaccine supply, both in Southern Nevada and nationwide. As a result, the vaccine is limited to those who have been recently exposed and those who are at elevated risk. As of the beginning of September, it is available at the Southern Nevada Health District, Huntridge Family Clinic, and The LGBTQ Center of Southern Nevada.
Finally, are there any monkeypox myths being shared out there that you’d like to ensure folks have the facts about?
I think there is an inaccurate perception that monkeypox is something that is only spread among men who have sex with men (MSM) and that being MSM means you are going to get monkeypox.
While it’s true the disease has gained a foothold in the MSM community, we have identified cases in children, household contacts, and people who are not MSM. While it’s important that those in high-risk groups should take extra precautions, it’s important for everyone to be aware that it’s out there.